Our Mission
We strive to offer our clients better control of their workers’ compensation programs by utilizing technologically advanced strategies and team-based, flexible problem-solving initiatives to achieve superior outcomes for our clients.

Who We Are
NCAComp, Inc. is a Third Party Claims Administrator for New York State workers’ compensation and disability claims. Since 1991, we have advanced and continuously evolved to serve different types of clients around the New York State area and across the United States. Moreover, our service offerings have increasingly diversified to provide our clients with the tools to manage every aspect of their workers’ compensation program.
Since its inception, NCA’s team has grown to 95 employees, who work together to save our clients money through the efficient administration of claims. We maintain a low case count so that our dedicated adjusters can focus on closing claims, effectively utilizing cost-saving programs, and properly administering benefits.
As of 2024, we’re proud to be a New York State Certified Minority and Women-Owned Business Enterprise.

Based on staff feedback, we are proud to have been named a Best Place to Work by Business Insurance in 2024 and 2025.



How We Work
Our specialists at NCA are constantly working to create the most technologically-advanced platform for claims management. This proprietary, in-house software not only allows for our adjusters to work smarter, but also for our clients to receive the reporting, results, and transparency they need to make fundamental program decisions.
Because of NCA’s diligent staff and advanced technology, we are able to save our clients millions of dollars a year. We track these savings through a detailed quality assurance program that ties into our incentive program for our employees. Through this program, our employees are able to share in the success of our clients, too.
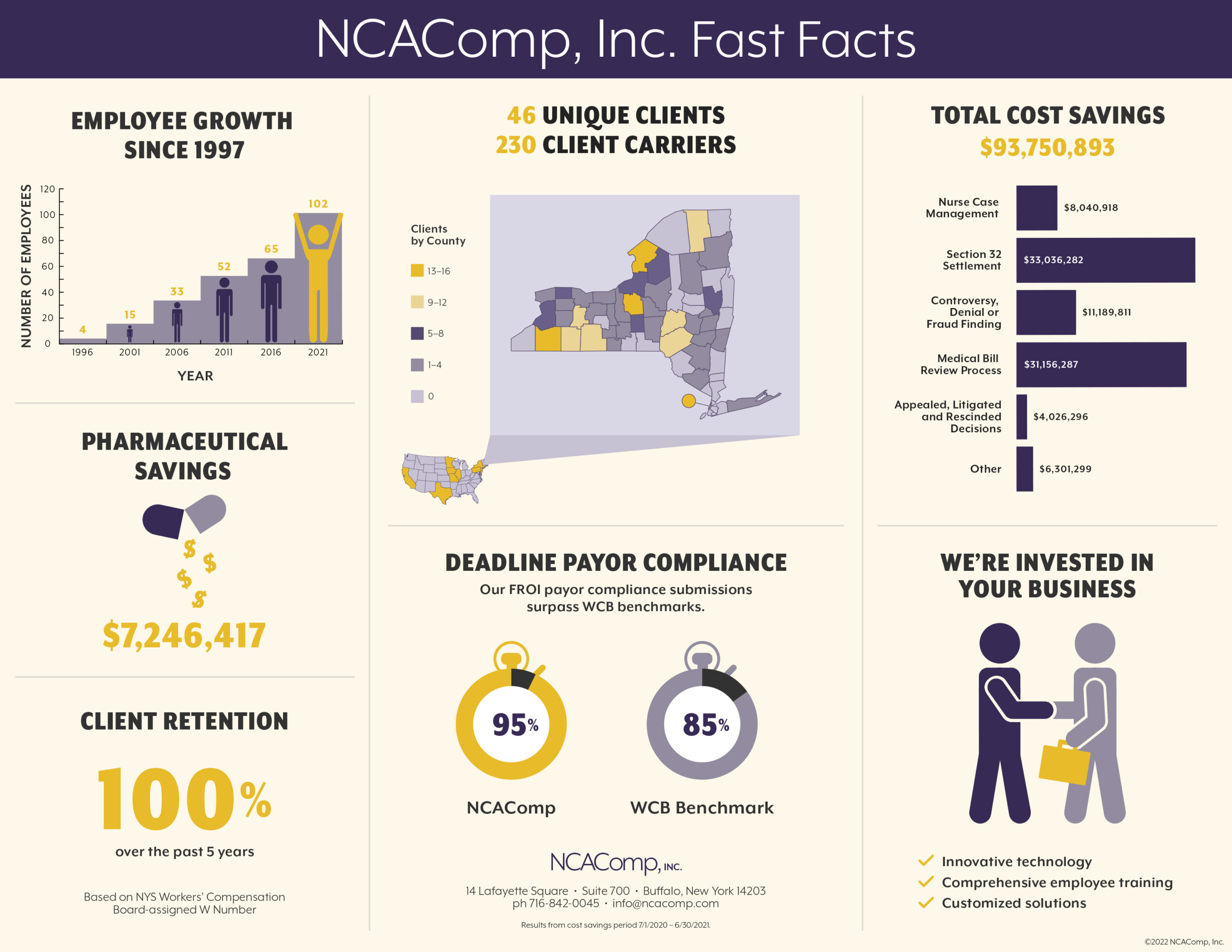
We are proud of what we do – and we have the facts to prove it.
See what we’re all about and download our Fast Facts for another
amazing year of growth.
